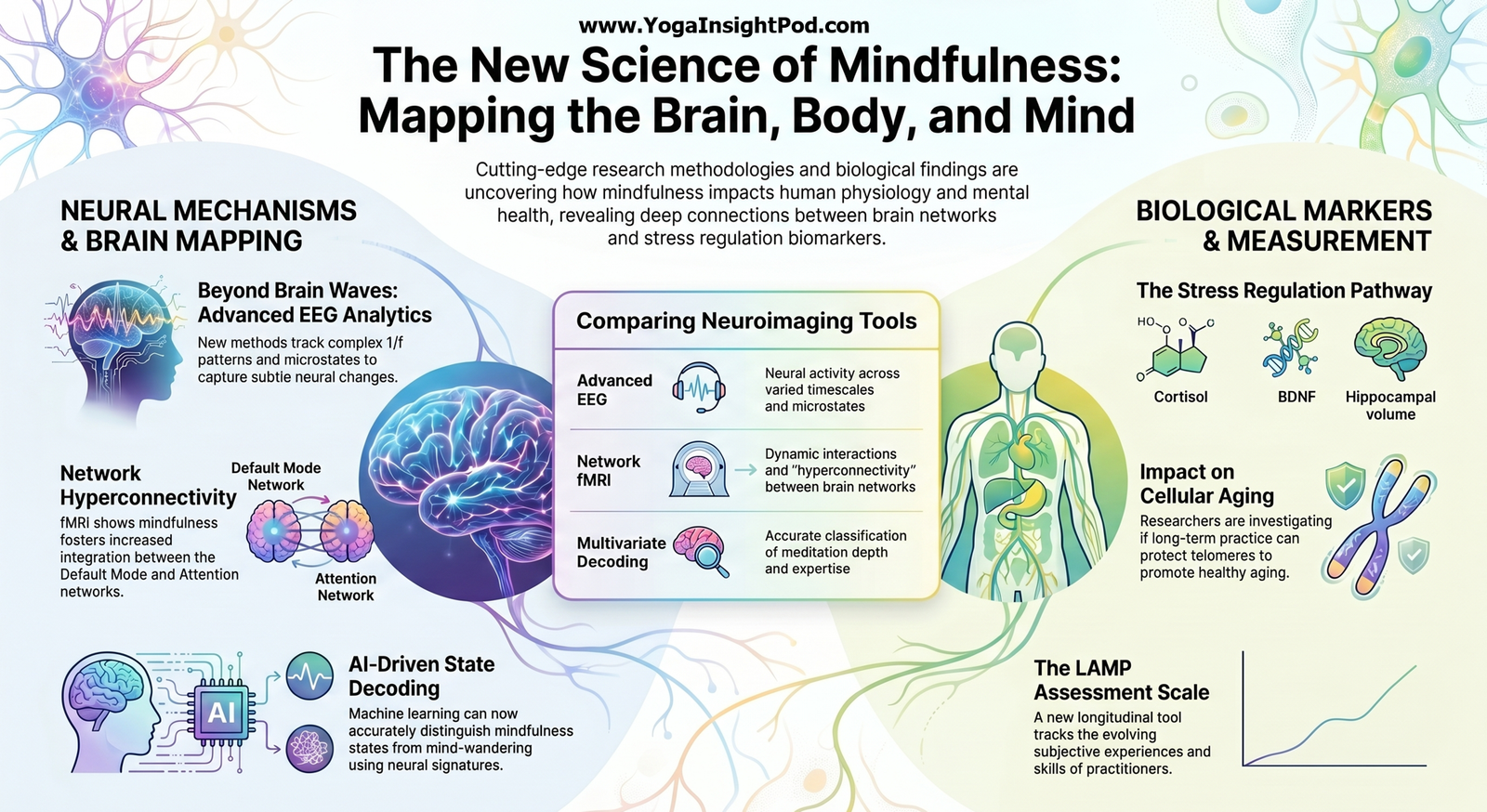
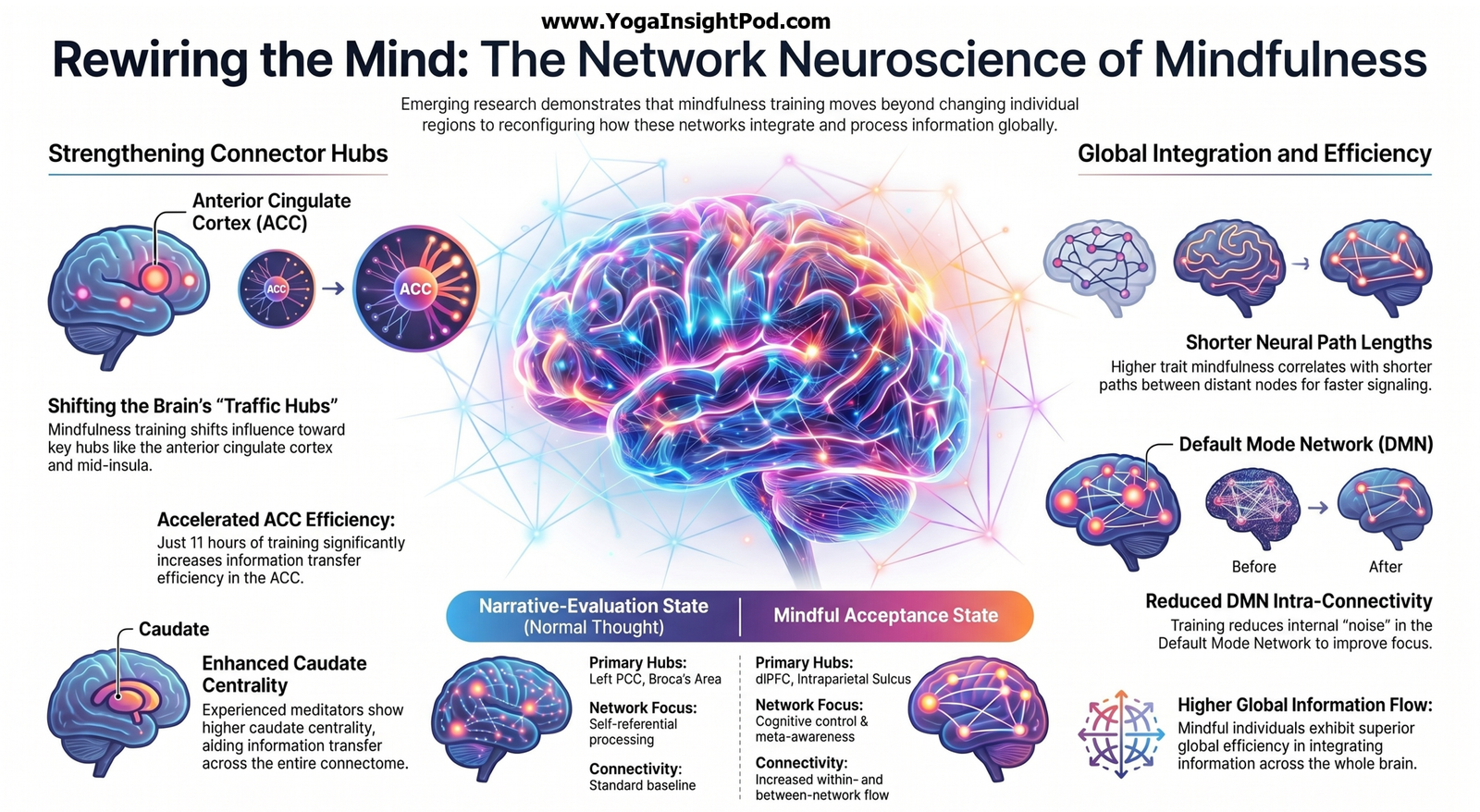
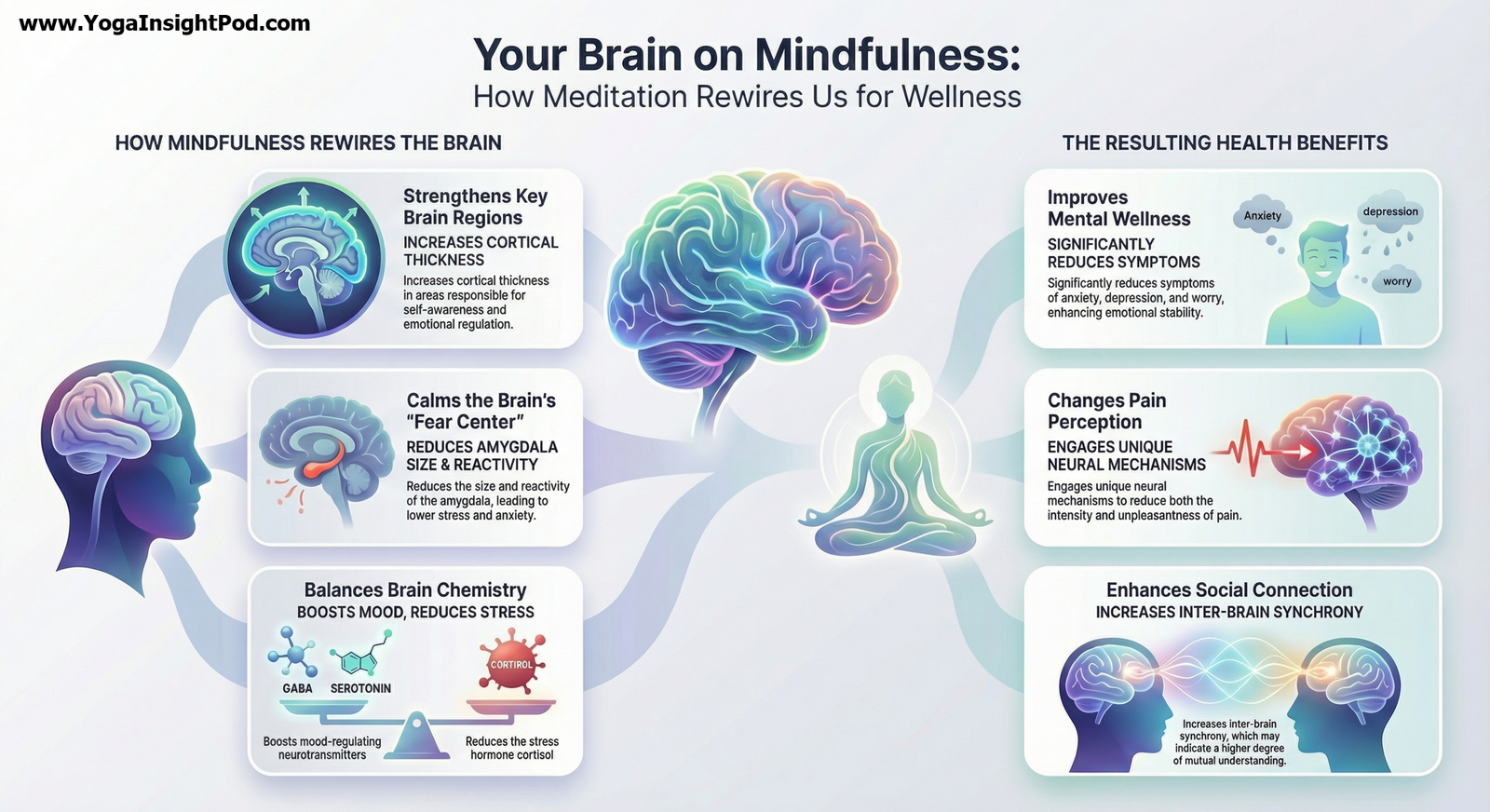
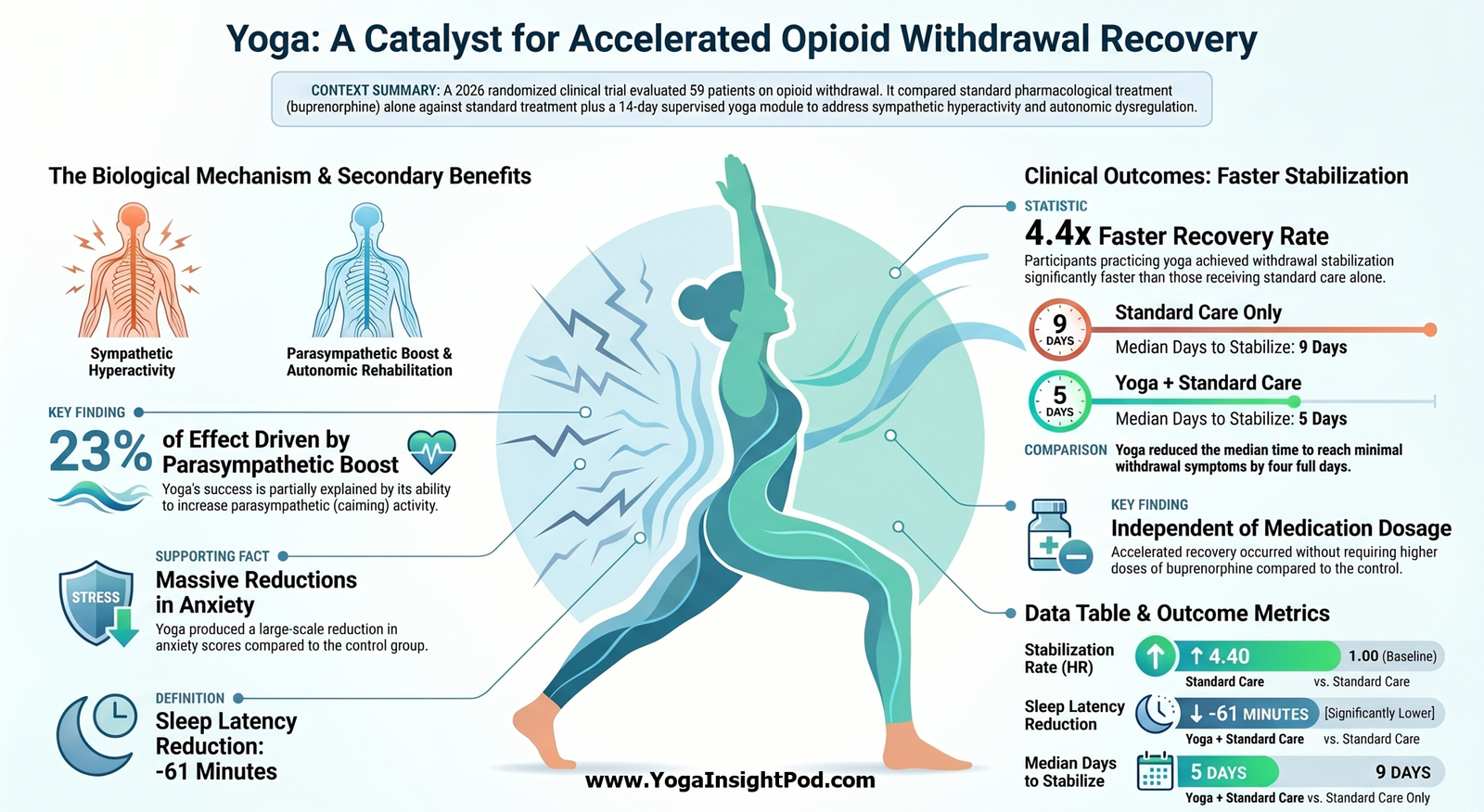
A JAMA Psychiatry randomized fMRI trial in adults with social anxiety disorder conducted at University of California Davis, Stanford University, and Temple University found that both cognitive behavioral group therapy and mindfulness-based stress reduction produce durable symptom improvements and strengthen prefrontal cingulate networks involved in reappraisal and acceptance. Subtle differences in how each treatment engages these circuits may underlie their distinct therapeutic mechanisms.
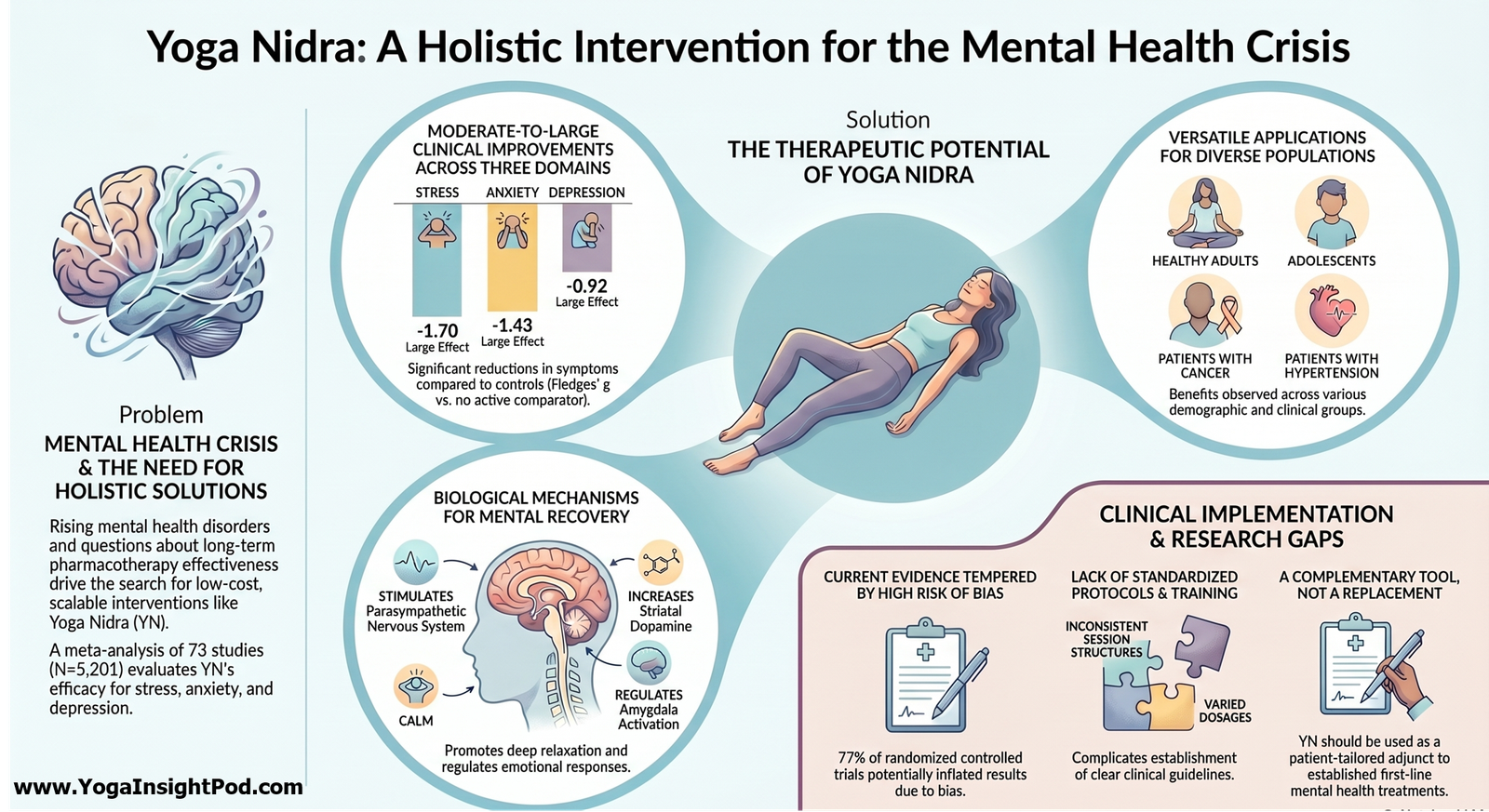
A 2021 randomized clinical trial in JAMA Psychiatry directly compared cognitive behavioral group therapy (CBGT) and mindfulness-based stress reduction (MBSR) in 108 unmedicated adults with generalized social anxiety disorder (SAD), looking not just at symptoms but at how each treatment reshapes emotion regulation brain circuits. Participants were randomized to 12 weeks of CBGT, MBSR, or a waitlist; both active treatments produced similar, substantial reductions in social anxiety and negative emotion that were maintained at 1 year follow up, with no significant differences between CBGT and MBSR on self reported distress when reacting to, reappraising, or accepting negative self beliefs.
Using fMRI during an autobiographical social-evaluative task, the researchers found that both therapies, compared with waitlist, increased activation in key cognitive and attention-regulation regions including dorsomedial and dorsolateral prefrontal cortex, dorsal anterior cingulate, ventrolateral prefrontal cortex, supramarginal gyrus, and thalamus when participants reappraised or accepted negative self beliefs. These overlapping neural changes suggest that, despite different therapeutic models, CBGT and MBSR converge on strengthening frontoparietal networks that support deliberate reappraisal and mindful acceptance.
The study also probed treatment-specific mechanisms: greater reappraisal related brain activation after CBGT, and patterns of acceptance-related responding after MBSR, were differentially associated with lower social anxiety one year later, hinting that CBT may exert its lasting impact more via cognitive reframing circuitry, while mindfulness may rely more on cultivating an accepting stance toward internal experiences. Overall, the findings support offering both CBT and mindfulness-based interventions as evidence based options for SAD, with each engaging slightly different, but partly shared, emotion-regulation pathways in the brain.